Temporomandibular Joint Syndrome (TMJ)
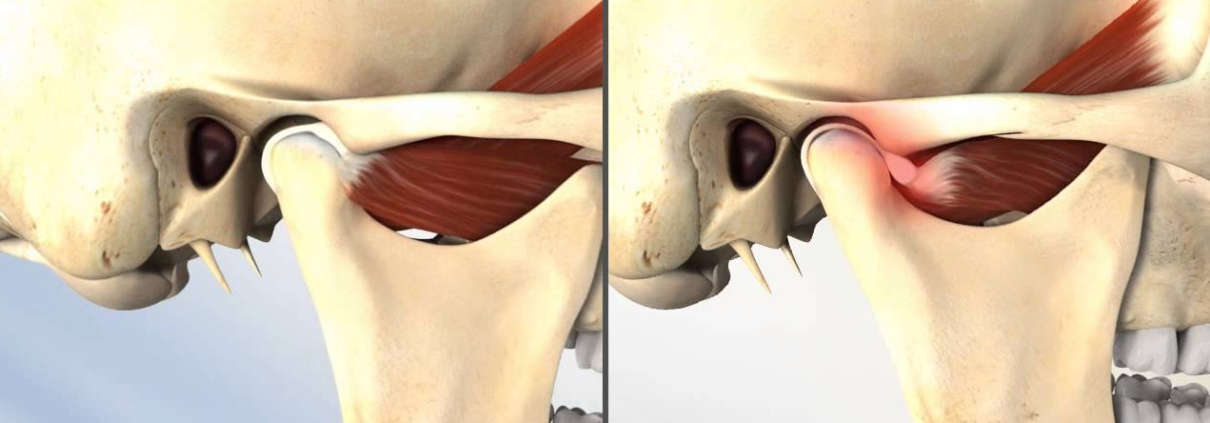
The temporomandibular joint is where the lower jaw meets the skull and consists of the rounded end of the lower jaw (the condyle), a disc, and the socket in the skull, along with the nerves and muscles used to mobilize the jaw. The action of the joint should be smooth but can be disturbed by structural abnormalities, inflammation, and trauma, as well as problems of nerve transmission. When the jaw is closed the disc and the condyle are in the socket. As the jaw opens the disc slides forward as does the condyle. This can be felt by placing two fingers just in front of the ears on the side of the face and opening the mouth. A smooth action suggests a healthy jaw; if one side moves more than the other, or if there is a jerky, popping action this suggests some pathology at work. Diagnosis of temporomandibular joint syndrome relies on a review of symptoms and functional scans of the joint to observe any skeletal, muscular, or nerve anomalies in the area.
Neck and jaw pain, along with pain radiating up to the head and down into the shoulders can be caused by temporomandibular joint syndrome/disorder. In this condition there can be acute and chronic nerve inflammation and structural anomalies. Pain may be uneven with both right-sided neck pain and left-sided neck pain experienced exclusively in some cases. As there are numerous nerves connecting the muscles of the face, neck, and jaw to the cervical spine some patients with temporomandibular joint disorder may even feel pain in the ears and the face.
Treatments for temporomandibular joint syndrome, also historically known as Costen Syndrome, will generally involved correction of the structural abnormality if present, alleviation of inflammation, and analgesics to relieve the patient’s pain. Physical therapy may be beneficial in some cases, along with neck and jaw exercises to correct the uneven muscle tone that can result from this disorder over many years.
Causes of Temporomandibular Joint Syndrome
The temporomandibular joint actually has two joints, allowing for rotation and translation (slide). As with any other joint in the body it is susceptible to degenerative disease, and simple wear and tear. Ankylosis, cervical spondylosis, cervical arthritis and arthritis in the jaw, dislocation, and trauma such as whiplash, can all cause temporomandibular joint syndrome. Developmental anomalies are also responsible for many incidences of the disorder as a structural asymmetry to the joint can cause dysfunction, pain, and an acceleration of degeneration. Problems with the condyle and the disc are frequently the cause of temporomandibular joint syndrome, with a variety of clicking, popping, and crepitus heard on movement of the joint.

Usually the temporomandibular joint does not have any nerve receptors on the surfaces of the bone and cartilage that contact each other. Instead, the joint relies on the pain signals from nerves in the surrounding soft tissues or the trigeminal nerve to alert it to an inappropriate and damaging movement that needs to cease. Improper signalling of these nerves may cause unnecessary pain and reduce the temporomandibular joint’s mobility. Inflammation of the trigeminal nerve, through trauma or infection can lead to constant chronic pain with acute flare ups. Ear ache (otalgia) is present in nearly half of those with temporomandibular joint syndrome (Tuz, 2003). Secondary otalgia is also caused in some cases by temporomandibular joint syndrome with treatment of this condition having benefits for the otalgia, tinnitus, and facial pain associated with the pathology (Sobhy, 2004, Ramirez, 2005).
Teeth can be a further cause of temporomandibular joint syndrome, with many patients developing their TMJ symptoms after the removal of their wisdom teeth. Grinding of the teeth, whether consciously or unknowingly whilst asleep, can cause the disorder, with the muscles of the jaw strained by the repetitive movement. Chewing gum excessively, or biting the nails, chewing pens, or eating tough foods frequently can also strain the jaw and lead to pain and reduced mobility.
Symptoms of Temporomandibular Joint Syndrome
Temporomandibular joint syndrome or disorder is characterized by acute or chronic pain of the jaw joint where the mandible connects to the skull. Patients may also experience referred pain in the head, neck, face, and shoulders. There can be both simple and complex symptomology observed in the condition, although usually more than one of the temporomandibular joint components is involved, such as the muscles, the nerves, the bones, and the blood vessels in the neck and jaw.
Significant impairment and pain may result from temporomandibular joint syndrome with the patient having difficulties eating through an inability to open the mouth fully, to chew properly, and to swallow. Weight loss may occur as the patient finds it too difficult and painful to eat. The presence of dental problems alongside temporomandibular joint syndrome is common, with wisdom teeth, gum disease, and
teeth grinding all contributing to the disorder. The patient may also notice a clicking or popping sound when opening or closing the mouth, or even a grating noise in some cases (known as crepitus). It is also possible for the jaw to be dislocated after stretching it out in an attempt to alleviate dental pain, such as the growth of wisdom teeth. The jaw may also slide out during sleep if the patient is resting on their side at an awkward angle.
Headaches and Ear Pains
Ear pain through swelling of nearby tissues is quite common, particularly first thing in the morning, and persistent ear pain may lead to tinnitus, and hearing loss as the inflammation causes permanent damage to the structures in the ear. Early morning headaches are another sign of temporomandibular joint syndrome, with some experiencing migraines with severe pain and nausea. The pain felt in the jaw may also be referred pain from other structures, or a sign of tension and stress.
Temporomandibular Joint Syndrome Diagnosis

Evaluating the presence of temporomandibular joint disorder usually involves careful palpation of the jaw joints at rest and in motion. Some physicians may tap on the teeth with a metal probe to assess the presence of any dental anomalies and pain. The patient is also likely to be asked to bite down on a wooden tongue blade and to report any incidence of pain whilst doing so. X-rays are taken whilst the jaw is both closed, and then open, to ascertain the precise problem. MRI and CT scans may be conducted if the x-ray does not elicit an observable skeletal anomaly as the problem may lie in the soft tissues, muscles, nerves, or blood vessels of the temporomandibular joint. Problems such as an excessively steep articular eminance may be highlighted through the use of scans, and present a clear therapeutic strategy to alleviate the patient’s temporomandibular joint syndrome symptoms.
Temporomandibular joint syndrome can be a result of numerous issues and crosses the lines separating medical specialties such as dentistry, neurology and orthopaedics. This may mean that a diagnosis is difficult to acquire as each profession may attempt to diagnose the problem in isolation of the other issues present. This has ramifications for the treatment of temporomandibular joint syndrome as it is no good just treating a patient’s dental issue when they also have complex nerve and muscular problems as part of their disorder.
The investigation of previous trauma, such as whiplash, contact sports injuries, and previous dental work or infections can provide clues as to the pathology of the syndrome. Assessing the patient’s sleeping habits may also prove illuminating as they may not know of a nocturnal teeth-grinding habit. Similarly, the physician will usually take care to observe any nervous habits such as nail-biting, lip or cheek chewing, or frequent use of chewing gum during the consultation as these can all contribute to the pain experienced in the disorder.
Temporomandibular Joint Syndrome Treatment
Treatments for temporomandibular joint syndrome vary according to the cause of the condition. If the teeth are the root of the problem then a dental surgeon may need to correct the issue through the removal of the offending wisdom teeth or other feature. Patients who have bridges may need to check that they are properly aligned as this can be the cause of a chronic strain on the muscles in the neck and jaw leading to temporomandibular joint syndrome. Mouth guards (occlusal splints) can be used if the patient grinds their teeth at night, although in some patients this actually increases the teeth clenching activity. The guards can be useful for preventing further loss of tooth enamel but should be monitored for any increase in the symptoms of temporomandibular joint syndrome. Mandibular Repositioning Devices (MORA) may be helpful in the short term to alleviate pain as a result of clicking on opening the mouth in those suffering from temporomandibular joint syndrome. Using these devices long-term is not recommended as they may substantially alter the position of the teeth causing irreversible complications. Instead, a patient who finds relief from the MORA may be offered a night-time only version consisting of a flat-plane bite plate.
Before commencing any more invasive procedures the dentist should investigate the potential cause of the problem and ascertain whether it is due to the patient having a para-functional jaw habit which is inciting the temporomandibular joint syndrome. The use of a nighttime biofeedback headband may help the patient to correct any actions precipitating the disorder. Actions other than grinding of the teeth can cause misalignment of the jaw, including lip or cheek biting, repetitive chewing habits, and aligning the lower jaw in an edge-to-edge bite.
Medications for TMJ
Medications such as analgesics and anti-inflammatories can provide relief from temporomandibular joint syndrome. However, as the pain is often associated with neurology these medications (such as acetaminophen and NSAIDs) may only provide short-term relief. Tricyclic antidepressants such as amitriptyline and nortriptyline have anti-muscarinic properties and are generally more effective at modifying pain than conventional analgesics.
Understanding how to help yourself

Another therapeutic course involves the use of biofeedback in order to re-teach the patient to use their misaligned jaw muscles correctly. A simple way of doing this is to draw a vertical line on a mirror and then observe the jaw relaxing during exhalation. Daily practice of watching the jaw relax in the mid-line can calm the symptoms as the jaw is gradually taught to realign. Gentle relaxation and stretching exercises should be discussed with the health care provider, as some may be inappropriate for every patient. The Feldenkrais Temporomandibular Joint Program can reduce chronic tension in the jaw, neck, face, and back by building on an understanding of human neurology. This may be able to reverse some of the habits that have led to the syndrome initially.
TMJ Surgery
Surgical replacement of the jaw joint(s) should be a last resort, with all other conservative treatment options explored first. Initial treatments should generally be reversible, i.e. causing no permanent structural alterations.

Arthrocentesis is a procedure that is performed under general anaesthetic and involves use of a saline and anti-inflammatory solution to wash out the temporomandibular joint. This may successfully break the cycle of inflammation and allow the body to commence healing. Some problems, however, are more intractable and require more permanent procedures such as disc replacement, disc repositioning, and joint replacement. Articular eminance recontouring is another procedure used
to correct a structural problem, which may be congenital, that causes excessive pressure on the condyle and disc. By reshaping the articular eminance so that there is more space between it and the condyle, the patient may find a significant reduction in the severity of their symptoms.
These procedures are known as arthroplasty and can be very successful in reducing or removing jaw pain and associated symptoms of temporomandibular joint syndrome. Complications of TMJ surgery include the usual risk of bleeding, swelling, pain, and infection. Arthroplasty also carries the risk of damage to the ears and facial nerves, and some patients may still feel pain after the surgery.
TMJ References
Ramírez, L.M., Sandoval, G.P., Ballesteros, L.E., (2005), Temporomandibular disorders: referred cranio-cervico-facial clinic, Med Oral Patol Oral Cir Bucal, Vol.10, S.1, pp.18-26.
Simmons, H.C. 3rd, Gibbs, S.J., (2009), Anterior repositioning appliance therapy for TMJ disorders: specific symptoms relieved and relationship to disk status on MRI, J Tenn Dent Assoc, Vol.89, No.4, pp.22-30.
Sobhy, O.A., Koutb, A.R., Abdel-Baki, F.A., Ali, T.M., El Raffa, I.Z., Khater, A.H., (2004), Evaluation of aural manifestations in temporo-mandibular joint dysfunction, Clin Otolaryngol Allied Sci, Vol.29, No.4, pp.382–5.
Tuz, H.H., Onder, E.M., Kisnisci, R.S., (2003), Prevalence of otologic complaints in patients with temporomandibular disorder, Am J Orthod Dentofacial Orthop, Vol.123, No.6, pp.620–3.